How can physical therapy help you reduce lower back pain?

Lower back pain will be experienced by most adults at some point in their lives. In fact, it is the most common musculoskeletal pain issue in adults that are seeking medical care. As many as 84% of all adults will have at least one episode of lower back pain sometime during their lives.1
Lower back pain that is muscular in nature will very often resolve in a matter of days or a few weeks with conservative treatment. This can include the use of NSAIDs (non-steroidal anti-inflammatory drugs) such as Ibuprofen or Naproxen to reduce inflammation, ice or heat, and stretching.
If an episode of lower back pain lasts more than 12 weeks or 3 months, then it will require more specific treatment. If lower back pain that has not resolved in this time frame then it is considered chronic in nature.
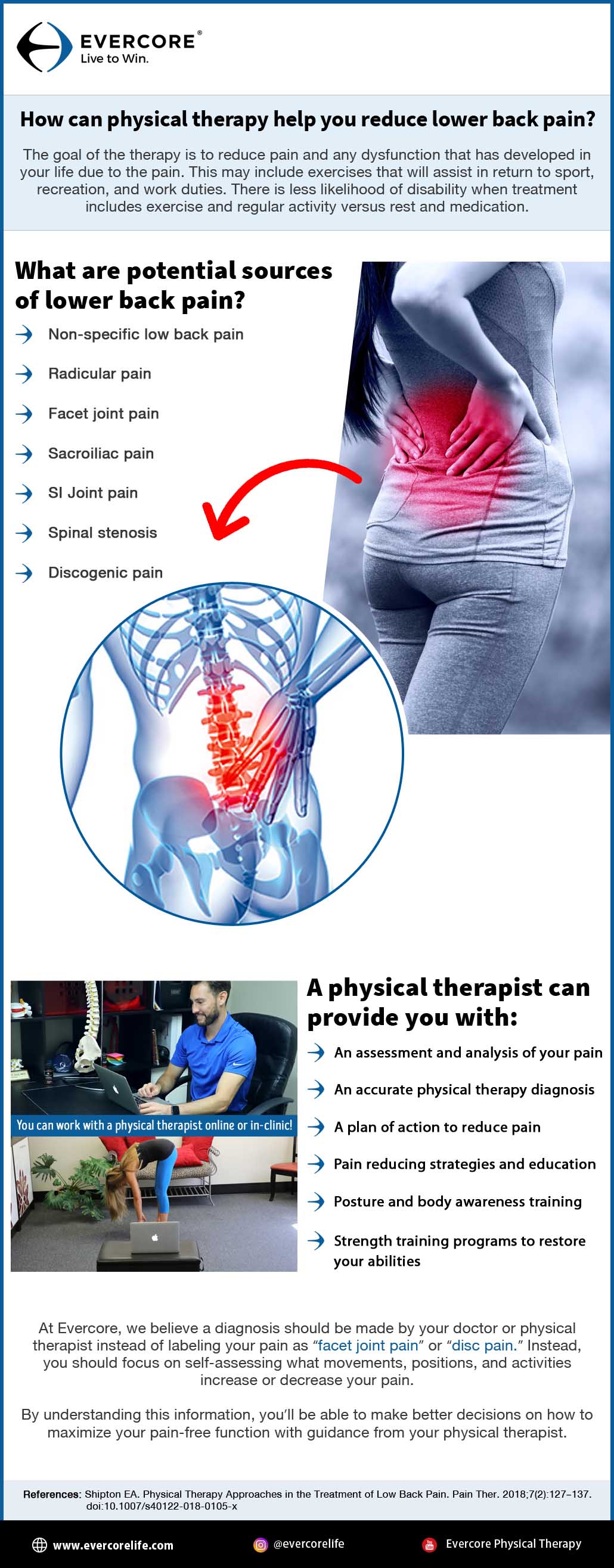
What are potential sources of lower back pain?
Low back pain is sometimes referred to as mechanical back pain. This simply means that the source of the pain is somewhere within the tissue of the bones of the spine, the discs, or the surrounding soft tissues of ligaments and muscles.2 Mechanical back pain can then be broken down into separate categories based on the tissue that is injured or affected.

1. Non-specific low back pain1
There are many times that a back pain diagnosis is considered non-specific, meaning that the reason for the pain is not clearly identified through testing. This is not necessarily a problem as treatment for the low back pain, even if the problem is not clearly defined, is very often successful.
Expensive testing can often be avoided in most individuals. When the pain lasts greater than 3 months and becomes chronic in nature, further work up or assessment may then be required to establish appropriate treatment.
2. Radicular pain1
Radicular pain is a pain that travels down the leg from the low back or from the buttocks. This pain is caused by an irritation of the nerve root that has exited the spine. It is most commonly seen when a disc herniation is present.
However, the pain most often comes from the inflammation of the nerve rather than the nerve being compressed by the herniated disc. This is why treatment for this with NSAIDS, time, and physical therapy can be successful. This is a good place to note that disc herniation alone is NOT the source of the radicular pain.
Studies have shown that when individuals who DO NOT experience any low back or leg pain undergo an MRI, a large percentage will have a herniated disc. It is a common misconception that the disc will have to be “fixed” in order for the pain to go away. This simply is not true in most cases. The symptoms will often resolve when the inflammation around the nerve root has lessened.

Radiculopathy is different from radicular pain in that it involves more than just a pain symptom. Radiculopathy involves the presence of altered sensation like tingling or numbness down the leg, muscle weakness, pain, and possibly bowel or bladder dysfunction.
The cause of radiculopathy is from either disc herniation or from stenosis or narrowing of the area where the nerve roots leave the spinal column. If radiculopathy is suspect then it will warrant further testing and treatment.
3. Facet Joint Pain1
The facet joints are on the back of the spinal column and are made up of the surface between two vertebrae that sit on top of each other. There is a facet joint on each side of the back of the vertebrae. The joints have close proximity to nerves in the area which gives rise to the pain that can come from this area of the spine.
Low back pain that is coming from the facet joints is found in about 30% of patients whose back pain has become chronic. Some studies show the percentage of people with facet joint pain to be lower. And some researchers believe that facet joint pain is cannot be distinguished from other types of lower back pain.

Those individuals that present with this type of pain will often complain of stiffness in their lower back. Their pain is worse with bending backward or extending their spine, side bending or rotating, and when walking up hill. Their point of pain is usually just off center of their spine where the joint is located. Some individuals will have leg pain as well which commonly is only in the thigh area of one or both legs.
4. Sacroiliac Pain or SI Joint Pain1
The SI joint is the surface between two bones of the pelvis; the sacrum and the two ilium bones. There are two SI joints, one on each side of the sacrum which is the lowest portion of the bones of the spine before the tailbone.
Pain from this area is likely inflammatory in nature. This can be from osteoarthritis in that joint, ligament strains surrounding the joints, or potentially from rheumatoid arthritis. Those with this type of pain will have pain directly over the area of the joint. The pain can be in only one joint at a time or in both.
This pain is worse with sitting or changing positions. It is often seen in women who are pregnant or breastfeeding because their ligaments are loose due to hormonal changes. It is also seen in those who have fallen or stepped incorrectly off to one side to cause a shift in the pelvic bones.
5. Spinal Stenosis1
Spinal stenosis is the narrowing of the space in the spinal column. The narrowing occurs most often in individuals in older age and occurs from degeneration of the spine over time. The narrowing causes there to be compression on the spinal cord and exiting nerves.
Symptoms are back pain in the center of the low back as well as leg pain that is worse with standing and walking, also known as claudication. Individuals with spinal stenosis also have other leg symptoms that can include tingling and muscle weakness.
6. Discogenic pain1
There are times when the back pain actually does stem from the intervertebral disc that sits between the two bones or vertebrae. This is often referred to as degenerative disc disease. Overtime the fluid filled disc will decrease in size and may even develop small tears in the outer portion of the disc. These changes can lead to chronic low back pain that may be accompanied with pain in one or both legs.
Low back pain assessment
With the many factors that are potential causes of low back pain it is vital that a thorough assessment is completed if the back pain has not resolved on its own. In our healthcare system, many people will begin with their primary care provider as the first step in medical treatment. A referral to physical therapy may likely follow.
A trained physical therapist will be able to complete an assessment that can likely determine which of the causes of low back pain are contributing to your symptoms even if imaging has not been performed.
Through a series of questions and analysis of your painful movements, your physical therapist can determine which treatments will best suit you. Different forms of exercise can assist with different types of lower back pain.

Can you and should you self-assess your lower back pain?
If you start to self-assess the source of pain with lower back pain, then you can start believing that you suffer from “facet joint pain” or “disc pain” when these may not be the real issues. Unfortunately, an incorrect self-diagnosis can lead to fear of exercise, unnecessary restrictions in activities, and other self-limiting beliefs that impair quality of life.
At Evercore, we believe a diagnosis should be made by your doctor or physical therapist instead of labeling your pain as “facet joint pain” or “disc pain.” Instead, you should focus on self-assessing what movements, positions, and activities increase or decrease your pain. By understanding this information, you’ll be able to make better decisions on how to maximize your pain-free function.
Physical therapy as a treatment for lower back pain
Once a physical therapist has determined which type of back issue is likely the cause of your pain, a plan of care will be established. This plan will include exercises that will be progressed during the rehabilitation sessions with the physical therapist as well as performed by you at home on a regular basis. The exercises will work toward normalizing soft tissue that has been altered in some way because of spasm, pain, or weakness.
The goal of the therapy is to reduce pain and any dysfunction that has developed in your life due to the pain. This may include exercises that will assist in return to sport, recreation, and work duties. There is less likelihood of disability when treatment includes exercise and regular activity versus rest and medication.3
Another key aspect of a physical therapy plan is education. The physical therapist will be able to share knowledge about an your lower back problems to help you better understand the reasons for the specific exercises you are asked to do. Understanding how you are helping yourself specifically through exercise can increase your follow-through with the home exercise program.
The physical therapist will educate you on proper body mechanics and postures for work and home duties. The education will also include ways you can prevent future episodes of back pain or how to manage them more quickly on your own, before you reach the chronic stage.

Seeking treatment from a physical therapist for back pain that is either acute or chronic in nature is an excellent first choice. When a person seeks medical imaging of x-rays and MRIs as part of an initial treatment plan they can end up spending 3 times more money than when they visit physical therapy initially. 4 The testing often leads to more testing and multiple appointments with physicians only to have the person ultimately end up in physical therapy later.4
If a “red flag” to physical therapy such as a spine fracture is suspected then a physical therapist will recommend that you return to your doctor for further diagnostic and medical testing.
Low back pain is not a cookie cutter diagnosis and therefore treatment needs to be guided by a healthcare professional. Through their skilled assessment, a physical therapist can establish an action plan to help you feel great again.
Why is Evercore your best option for lower back pain recovery?
At Evercore, we use a specialized process to diagnose your lower back pain called the McKenzie Method. The McKenzie method is framework used by physical therapists to accurately determine the best action plan to reduce and prevent lower back pain.
The McKenzie method can be done online or in-clinic through a series of questions specific to your situation and by an analysis of your painful movements. Our physical therapists will monitor your response to these specific movements to determine what exercises to do and the order in which you should do them over the span of 2-4 weeks to reduce your lower back pain.
The McKenzie Method works well for both recent and chronic lower back pain that has lasted more than 3 months and it’s a great approach if no other treatments have helped you.